Child Neurology and Neurodevelopmental Disabilities Residency Training Programs | Research & Innovation
Spanning basic, clinical, and translational investigation, the research program in neurology at Boston Children’s Hospital is the largest at a pediatric facility in the world. Other rich neuroscience opportunities are close elsewhere on our campus and with collaborating institutions such as Harvard and MIT.
Boston Children’s offers child neurology residents almost limitless opportunities to engage in basic and translational neuroscience, participate in neurology clinical trials, and collaborate with cognitive neuroscience investigators.
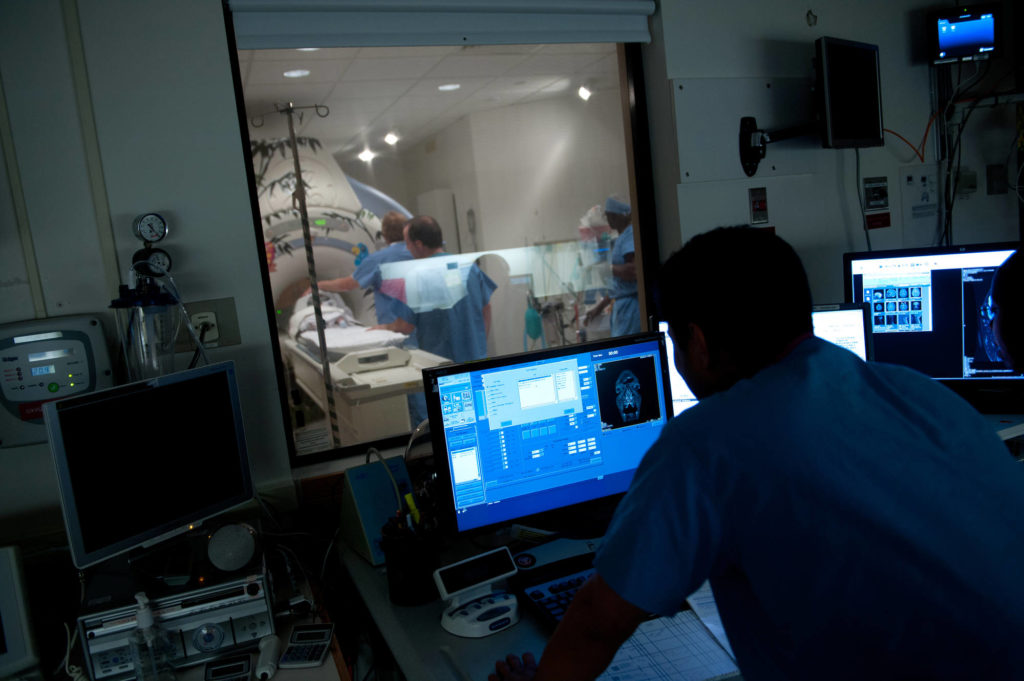
Research in the Department of Neurology
Research training is supported by an R25 grant, a T32 grant from the National Institute of Neurologic Disorders and by Stroke (NINDS), and a T32 grant from the National Institute of Mental Health.
Neurology residents can participate in a wide range of clinical trials, often in collaboration with basic scientists and clinicians in other departments and institutions.
Collaborating with researchers across Boston Children’s, we have access to a wide range of tools: genome editing, zebrafish drug-screening platforms, neural stem cell assays, advanced neuroimaging, proteomics, and many more. Many of our residents go on to complete postdoctoral research fellowships here after completing their clinical training.
Research around our campus
Just a block from the main hospital, the multidisciplinary F.M. Kirby Neurobiology Center has some 20 labs investigating all aspects of nervous system development with the goal of improving care and training the next generation of physicians and scientists in basic and translational neuroscience.
Down the street, the Laboratories of Cognitive Neuroscience are investigating brain and cognitive development in both typically developing infants and children and those diagnosed with or at risk for various developmental disorders.
Through our National Institutes of Health-funded Intellectual and Developmental Disabilities Research Center (IDDRC), residents also have access to other Longwood medical area scientists, as well as neuroscience seminars given by visiting neuroscientists from around the world.
Research beyond Boston Children’s
Next door at the Harvard Medical School’s Department of Neurobiology, residents can collaborate with scientists exploring the interactions between genetics and neuronal activity. Across the Charles River in nearby Cambridge, opportunities abound to collaborate with scientists at Massachusetts Institute of Technology (MIT). Boston Children’s has regular partnerships with MIT’s Department of Brain and Cognitive Science, the McGovern Institute for Brain Research, the Picower Center for Learning and Memory, and The Broad Institute.
Research support
The Neurology Department provides staff support to help residents in their research development, including preparing research proposals and study designs, and reviewing case reports and publications. Additionally, the Boston Children’s Hospital Clinical Research Program aids residents with grants, study protocols, case report forms, surveys, research databases, data or project management, data analysis, and education in clinical research methods and practice.
Basic and Translational Research staff
- Todd Anthony, PhD: Genetic dissection of neural circuits that control stress-induced behavioral states
- Larry Benowitz, PhD: Optic nerve regeneration and CNS reorganization after injury
- Chinfei Chen, MD, PhD: Synaptic plasticity
- Michael Crickmore, PhD: Neurobiology of motivational states
- Michael Do, PhD: Regulation of physiology and behavior by light
- Elizabeth Engle, MD: Congenital eye movement disorders
- Michela Fagiolini, MD: Experience-dependent visual plasticity, neurodevelopmental disorders, including Rett syndrome
- Gwenaelle Géléoc, PhD: Functional development of sensor hair cells in the inner ear
- Xi He, PhD: Cell-cell communication; early nervous system development, Wnt family of secreted morphogens and signaling; cancer, skeletal and neurologic diseases
- Zhigang He, PhD, BM: Axon regeneration
- Takao Hensch, PhD: Critical periods in brain development
- Jeffrey Holt, PhD: Molecular basis of sensory signals in hearing and deafness
- Karl Koehler, PhD: Development and regeneration of peripheral sensory systems
- Gabriel Kreiman, PhD, MSc: Computations in the brain and the functional architecture of neuronal circuits
- Wei-Chung Allen Lee, PhD: understanding the organizational principles that underlie information processing in neural circuits through the application of “functional connectomics” to discover the relationship between circuit structure and function in the Drosophila and rodent brain.
- Jonathan Lipton, MD, PhD: Circadian rhythms, neurological disease, translation
- Heather Olson, MD, PhD: Epilepsy genetics
- Scott Pomeroy, MD, PhD: Molecular and cellular biology of brain tumors
- Paul Rosenberg, MD, PhD: Physiology and pathophysiology of glutamate transporters in the central nervous system; molecular mechanisms of brain injury; mechanisms of homeostatic sleep regulation
- Alexander Rotenberg, MD, PhD: Noninvasive brain stimulation; epilepsy; traumatic brain injury
- Mustafa Sahin, MD, PhD: Neuronal wiring and neurological disease
- Thomas Schwarz, PhD: Neurotransmitter secretion, membrane trafficking, synapse development, axonal transport, Parkinson’s disease
- Judith Steen, PhD: Neurodegenerative diseases, proteomics and bioinformatics
- Beth Stevens, PhD: Neuron-glia signaling, synapse development, plasticity
- Xin Tang, PhD: Understanding brain function and dysfunction from model to mechanism to medicine
- Hisashi Umemori, MD, PhD: Wiring the functional brain
- Clifford Woolf, MB, BCh, PhD: Pain, formation of neural circuits, regeneration
Clinical research: A sampling of current studies
Boston Children’s is a fulcrum for neurology research. We are a member site in two NIH consortia for clinical trials: NeuroNEXT and NIH StrokeNet. Below is a selection of some of our other ongoing clinical research studies.
- Genetics of severe early onset epilepsies: This long-term study, led by Annapurna Poduri, MD, seeks to identify genetic alterations that cause severe early onset epilepsies, focusing on epileptic encephalopathies and Ohtahara syndrome in particular, with the goal of improving diagnosis and treatment.
- Rett syndrome: The Rett Syndrome Research Program at Boston Children’s Hospital, led by David Lieberman, MD, PhD, and Mustafa Sahin, MD, PhD, is committed to advancing our understanding of Rett syndrome and MECP2-related disorders by conducting research studies for patients with these rare neurodevelopmental disorders. In addition to offering multiple interventional clinical trials, we are also an active member of the NIH-sponsored Rett & Related Disorders Natural History Study and offer a new innovative biomarker study with two investigational devices that can track motion, breathing, and sleep of subjects through the collection of biometric, physiologic, and electronic clinical outcome assessment data to be used for future clinical trials.
- CDKL5 deficiency disorder: Boston Children’s Hospital’s CDKL5 Center of Excellence (COE), led by Heather Olson, MD, offers a comprehensive clinical care program dedicated to the care and evaluation of children and adults with CDKL5 deficiency disorder (CDD). The BCH COE enrolls patients in our clinic-based research program designed in collaboration with the other COEs and in the newly launched NIH UO1 funded International CDKL5 Clinical Research Network. We also have a strong collaborative network of researchers for translational and basic science CDKL5 research, which can be done in parallel with studies in our clinical center, including several interventional clinical trials.
- PTEN hamartoma tumor syndrome (PHTS): The Multidisciplinary PTEN program, led by Siddharth Srivastava, MD, in collaboration with the Developmental Synaptopathies Consortium, is conducting a Phase I/II clinical trial of the mTOR inhibitor, everolimus (Afinitor, Novartis Pharmaceuticals) in children and adolescents with PTEN mutations (U54NS092090). The primary aim of the study is to evaluate the safety of everolimus in this population of patients. Secondary outcomes include the short-term efficacy of everolimus on neurocognition and behavior, electrophysiological responses, dermatological features, and the microbiome of individuals with PTEN mutations.
- Pediatric Status Epilepticus Research Group (pSERG): pSERG is an international consortium coordinated out of Boston Children’s Hospital and led by Dr. Tobias Loddenkemper. This consortium is developing a registry of refractory status epilepticus episodes with the goal of investigating outcomes of prolonged seizures that are resistant to at least two lines of antiepileptic rescue medications.
- Tuberous sclerosis complex (TSC): The Multi-Disciplinary Tuberous Sclerosis Program, led by Mustafa Sahin, MD, PhD, is currently conducting a clinical trial of the antiepileptic vigabatrin (Sabril, Lundbeck Pharmaceuticals). The primary objective of the study is to test whether early treatment versus delayed treatment with vigabatrin in infants with TSC will have a positive impact of developmental outcomes at 24 months of age. A second objective is to determine if early intervention will prevent or lower the risk of the child developing infantile spasms and refractory seizures
- Duchenne muscular dystrophy (DMD): The Neuromuscular Program at Boston Children’s Hospital, led by Basil Darras, MD, is conducting a Phase III study of Golodirsen and Casimersen (Sarepta 4045-301 and 4045-302), two exon-skipping drugs with the aim to increase production of dystrophin protein in boys with DMD. Another phase II study is investigating the drug Pamrevlumab by Fibrogen Inc. in the hopes that it will slow muscle degeneration in boys with DMD. Lastly, a phase III study by Catabasis Pharmaceuticals is investigating the use of Edasalonexent in boys with DMD to see if it could be a viable replacement for steroid therapy, with reduced negative side effects.
- Spinal muscular atrophy (SMA): The Spinal Muscular Atrophy Program at Boston Children’s Hospital is led by Basil Darras, MD. His program was part of phase I , II, and III trials testing the safety and efficacy of Nusinersen or Spinraza, which was the first FDA-approved treatment for all types of SMA. Spinraza works by altering the splicing of the SMN2 gene, leading to the increased production of fully functional SMN protein. We continue to follow our original trial patients through an extension protocol. Biogen, maker of Spinraza, is starting a new study to test higher doses of Spinraza. Our program is also participating in the phase II and III trials of an oral small molecule, Risdiplam by Roche, that is also designed to alter the splicing of the SMN2 gene. These studies, Firefish and Jewelfish studies, led to Risdiplam being approved by the FDA in August 2020. Additionally, we have participated in AveXis Inc.’s, gene therapy for SMA type I patients (STR1VE), and SMA Type II patients (STRONG) using an AAV9 virus vector to deliver the SMN1 gene. STR1VE delivers the medication intravenously, and STRONG delivers the medication intrathecally. This gene therapy was FDA approved as Zolgensma, via IV administration for patients under 2. Lastly, we have started the TOPAZ trial, sponsored by Scholar Rock Inc., which is investigating a myostatin inhibitor, a muscle growth inhibitor to be used in combination therapy with other SMA therapies to improve muscle strength. The SMA Program also has an ongoing natural history study and is collecting specimens for a biorepository, which are sponsored by the charitable foundation, Cure SMA.
- Neonatal seizures: Janet Soul, MD, of Boston Children’s Fetal-Neonatal Neurology Program, is conducting a clinical trial directed at controlling neonatal seizures with bumetanide. Bumetanide is a diuretic that investigators at Boston Children’s and Massachusetts General Hospital have shown to lower chloride levels in the newborn brain, making neurons more responsive to GABA activation.
- Neurofibromatosis and pediatric brain tumors: Nicole Ullrich, MD, PhD, Director of Neuro-Oncology, is a founding member of a national collaborative group currently conducting a series of clinical trials in patients with neurofibromatosis. Recent trials have included testing the MEK inhibitor binimetinib and Cabozantinib in neurofibromatosis type 1 (NF-1) and bevacizumab and crizotinib for vestibular schwannomas in NF-2. Ullrich was national study chair for a randomized, placebo-controlled trial of modafinil to reverse cognitive deficits in survivors of pediatric brain tumors through the Children’s Oncology Group. She is leading a study that uses memantine to prevent cognitive decline related to radiation for primary brain tumors in children.
- Advanced seizure tracking and warning systems: Seizures frequently are not identified by patients and families. This trial, led by Tobias Loddenkemper, MD, tests novel, portable epilepsy monitoring sensors and tools that can detect seizures by means of autonomic nervous system features, patient movement, and other vital signs and parameters. The devices allow for rescue measures and tracking of less severe seizures and treatment responses, and may help patients gain better control over seizures.
- Angelman syndrome: The purpose of this study conducted by Alexander Rotenberg, MD, PhD (PI: Neurology), and Wen-Hann Tan, MD (co-I: Genetics & Genomics), is to evaluate the reliability and validity of select neurobehavioral assessments and EEG biomarkers as endpoints for future clinical trials in children and adults with Angelman syndrome (AS). This multisite study is sponsored by Roche Pharmaceuticals.
- Absence seizures: Alexander Rotenberg, MD, PhD. is conducting this study to validate a software solution for detecting absence seizures with wearable and clinical EEG systems. This project is both retrospective and prospective in nature, and it is sponsored by Epihunter NV in collaboration with the Epilepsy Foundation.
NIH training opportunities
The Department of Neurology at Boston Children’s is fortunate to hold three institutional NIH training grants. We have held an Institutional National Research Service Award for many years, which supports four scientists and/or physician/scientists as fellows each year. The award (T32 NS007473 Developmental Neurology; renewed 7/2021 with six slots per year; multi-PI Tom Schwarz and Elizabeth Engle) supports primarily bench laboratory research in developmental neurobiology. A total of 22 training slots have been awarded since 2015.
The most recently awarded training grant (T32 MH112510 Translational Post-doctoral Training in Neurodevelopment; start 7/2017; multi-PI Mustafa Sahin and Charles Nelson) is quite novel. It is designed to provide promising post-doctoral investigators (MD, PhD, or MD/PhD) with advanced training in essential translational topics ranging from preclinical considerations through implementation of clinical trials for individuals with a range of neurodevelopmental disorders. The program provides trainees with research experiences ranging from preclinical and cognitive neuroscience labs through clinical trial involvement in neurodevelopmental disorders.
Since 2010, the department has jointly held a NINDS R25 training grant with the Department of Neurology at Beth Israel Deaconess Medical Center (R25 NS070682 CH/BIDMC/Harvard Medical School Neurology Resident Research Education Program; Renewed 7/2020; multi-PI Scott Pomeroy, MD, PhD, and Clifford Saper, MD, PhD). This unique training grant provides research funding for six months during neurology residency which can be extended up to 30 months with a requirement to submit an individual NIH K-award application, a program that facilitates the transition from residency to research fellowship/emergence as an independent investigator. Awardees are closely monitored with multiple mentors. The NIH hosts an annual meeting of all R25 awardees across the country on the NIH campus. Each applicant submits a research proposal to NINDS for a project funding decision in the fall of their penultimate year of residency for funding starting in the final year. The department currently has several active awardees. The table below summarizes funded residents from the inception of the program:
R25 resident funding
Former trainees
| Trainee name | Mentor | Current position |
| Soma Sengupta, MD, PhD | Pomeroy | Associate Professor of Neurology and Rehabilitation Medicine, Division Chief Neuro-oncology, Professor, University of North Carolina |
| Christopher Elitt, MD, PhD | Rosenberg | Instructor in Neurology, Harvard Medical School, Boston Children’s Hospital |
| Peter Davis, MD | Sahin | Instructor in Neurology, Harvard Medical School, Boston Children’s Hospital |
| Danielle Pier, MD | Soul | Instructor in Neurology, Harvard Medical School, Massachusetts General Hospital |
| Christopher Yuskaitis, MD, PhD | Poduri | Associate Medical Director, Tekada |
| Bhooma Aravamuthan, MD, DPhil | Rutkove, Robinson and Young | Assistant Professor of Neurology, Washington University in St. Louis |
| Ervin Johnson, MD, PhD | Rotenberg | Pediatric Epileptologist, Neurology Centre of Toronto, Canada |
| Kellen Winden, MD, PhD | Sahin | Instructor in Neurology, Harvard Medical School, Boston Children’s Hospital |
| Melanie McNally, MD | Staley | Child Neurology Research Fellow, Massachusetts General Hospital |
| Darius Ebrahimi-Fakhari, MD, PhD | Sahin | Assistant Professor, Harvard Medical School, Boston Children’s Hospital, Assistant Professor and Director, Movement Disorders Program |
| Diane Shao, MD, PhD | Walsh | Instructor, Harvard Medical School, Boston Children’s Hospital |
| Milena Andzelm, MD, PhD | McCarroll Eggan | Instructor, Harvard Medical School, Boston Children’s Hospital |
Current trainees
| Trainee name | Mentor | Current position |
| Divya Jayaraman, MD | Beggs | Child Neurology Research Fellow, Boston Children’s Hospital |
| Alisa Mo, MD | Walsh | Child Neurology Research Fellow, Boston Children’s Hospital |
| Catherine Salussolia, MD, PhD | Sahin | Child Neurology Research Fellow, Boston Children’s Hospital |
