Child Neurology and Neurodevelopmental Disabilities Residency Training Programs | Career Development
Whether your career goal is general clinical neurology, subspecialty neurology, research. or a mix, the Child Neurology Residency Training Program provides strong support and guidance on grants, fellowships, research projects, and more.
Current careers of former residents
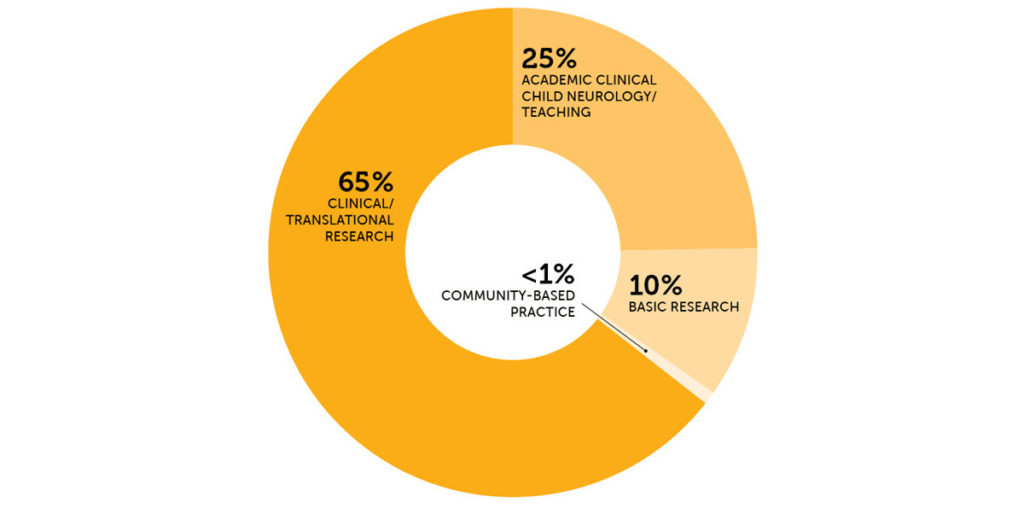
Mentoring and advising
Mentoring and advising is central to our program, and we employ a multi-tiered approach to ensure residents are accessing the best resources to reach their individual goals.
First, each resident forms a close relationship with the program director, Miya Bernson-Leung, MD, EdM, and the associate program director, Molly Wilson-Murphy, MD. Each week, the residents meet with Drs. Bernson-Leung or Wilson-Murphy for general conversation about residency. In addition, Drs. Bernson-Leung and Wilson-Murphy host office hours so that residents can pop by informally as needed. Finally, each resident has formal sessions twice annually to review their residency progress.
In addition, residents work closely with department chair Scott Pomeroy, MD, PhD, and associate program director for academic mentoring, Caitlin Rollins, MD, SD, throughout their training to develop their career goals and mentoring team. In the first year, residents begin meeting with Drs. Pomeroy and Rollins in coordination with residency program leadership to discuss career goals and existing mentors. The team works closely with each individual to ensure that they are connected to the breadth of opportunities at Boston Children’s Hospital, as well as the rich network of resources in surrounding institutions. Over time, as a resident’s interests become more established, Drs. Pomeroy and Rollins ensure that each resident has the breadth of expertise needed to help guide them into a research or career interest area. The team provides advice on how to get started with a project, as well as on planning for fellowships and faculty positions. These meetings continue throughout the second and third years, so that residents can receive graduated guidance on their research progress and career development. Biannual academic retreats provide further opportunities for mentorship and career development.
All residents have access to advisors in the Department of Neurology who match their clinical and/or research interests. Residents and their advisors typically formally meet biannually. Advisors develop a personal relationship with the resident, provide career guidance and mentorship, advocate for the resident to facilitate the resident’s professional development, and serve as a resource in personal and professional decision-making.
A sample of clinical and research fellowships chosen by recent graduates:
- behavioral neurology
- clinical neurophysiology and epilepsy/EEG
- developmental neuropharmacology
- electromyography
- neurogenetics
- movement disorders
- neuro-oncology
- pediatric sleep
